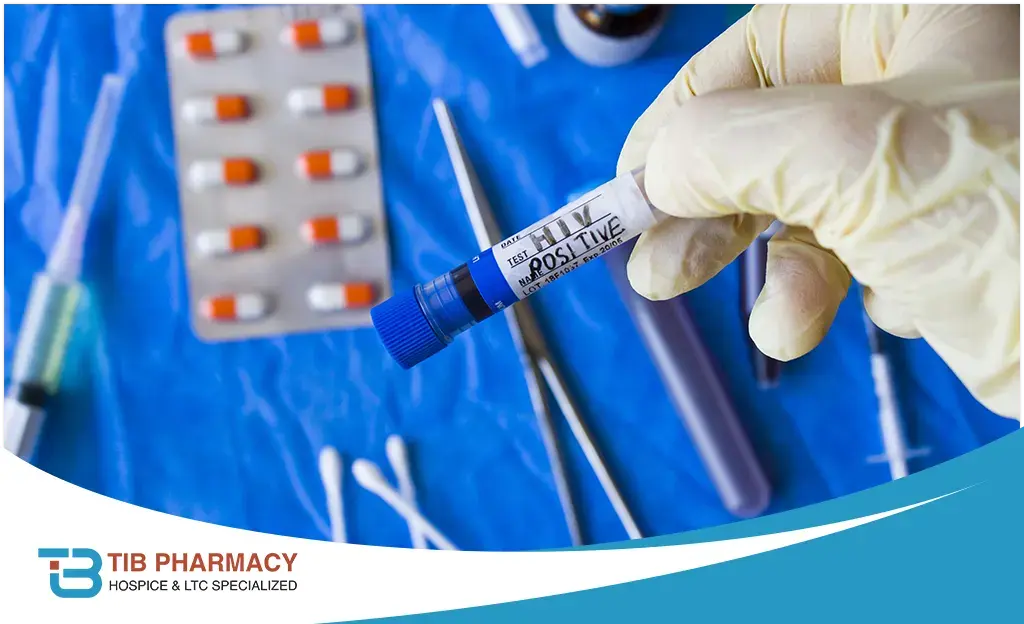
Long-term care facilities are crucial in providing support and medical care to people with chronic conditions like HIV. Antiretroviral therapy (ART) has transformed HIV from a once-fatal disease into a manageable chronic illness due to advances in medical science. As people with HIV live longer, it becomes essential to address the unique challenges of HIV medication management in long-term care settings. This article examines the complexities, considerations, and strategies for providing optimal care to HIV-positive long-term care facility residents.
Challenges in HIV Medication Management
Complex Medication Regimens: HIV treatment frequently involves a combination of multiple medications consumed at specific times and conditions. It can be challenging for residents and caregivers to adhere to a strict regimen, leading to concerns about missed doses and potential drug resistance.
Drug Interactions and Comorbidities: Many HIV-positive patients may have additional medical conditions requiring different medications. Managing potential drug interactions and ensuring HIV medications are compatible with other treatments is essential for preventing adverse effects and preserving overall health.
Stigma and Privacy: HIV is still associated with stigma, which can influence the propensity of residents to disclose their status or adhere to medication schedules. Providing a secure and nonjudgmental environment is essential to encourage open communication and medication adherence.
Cognitive Impairment: Some inhabitants of long-term care may experience cognitive decline, making it difficult for them to remember their medication schedules and adhere to complex instructions.
Strategies for Effective HIV Medication Management

Individualized Care Plans: Develop individualized care plans that consider the medical history, HIV treatment regimen, and potential medication interactions of each resident. Regularly review and update these plans as the health requirements of resident’s change.
Synchronization of Medication Schedules: Synchronize medication schedules to simplify administration and enhance adherence. This method can also facilitate the coordination of HIV medication dosage with other essential medications.
Support for Adherence Programs: Implement adherence support programs, such as medication reminders, pill organizers, and education sessions for residents and their caregivers. These programs can enable residents to participate in their treatment actively.
Staff Education and Training: Provide facility staff with comprehensive training on HIV, its treatment, and the significance of confidentiality. This education can reduce stigma, enhance communication, and ensure the appropriate administration of medication.
Regular Monitoring and Communication: Establish a system for ongoing monitoring of the health of residents, including assessments of viral burden and CD4 cell count. Encourage residents, caregivers, and healthcare providers to communicate openly to promptly address concerns.
Recognize the psychological effects of living with HIV and provide access to mental health services and support groups. A holistic approach to treatment can improve overall health and medication compliance.
Managing HIV medications in contexts of long-term care requires a multidimensional approach that addresses medical, psychological, and social factors. Long-term care facilities can ensure that residents with HIV receive the best possible care, improve their quality of life, and effectively manage their chronic condition by customizing care plans, providing support programs, and cultivating an environment without stigma. Adapting and enhancing HIV medication administration in long-term care settings will require continuing education and collaboration among healthcare providers, caregivers, and residents as medical advances continue.
Understanding HIV and its symptoms can be a complicated process. At TIB Pharmacy, we offer you a compassionate and caring ambiance where all your health-related issues are taken sincerely. Our professionals are always there to help. For more information visit www.tibpharmacy.com.
